Osteoporosis • Bone health-various aspects-
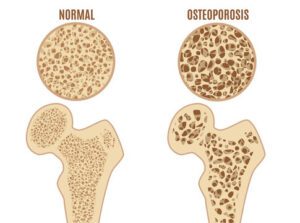

Osteoporosis is a condition characterized by weakened bones, making them more susceptible to fractures. It occurs when the body loses too much bone, makes too little bone, or both. Bones become porous and brittle, often resulting in fractures, especially in the hip, spine, and wrist.
Maintaining good bone health is crucial in preventing osteoporosis. Here are some tips:
- **Nutrition:** Ensure an adequate intake of calcium and vitamin D. Calcium-rich foods include dairy products, leafy green vegetables, and fortified foods. Vitamin D helps the body absorb calcium and is obtained from sunlight exposure and foods like fatty fish and fortified products.
- **Exercise:** Regular weight-bearing and muscle-strengthening exercises help maintain bone density and strength. Activities like walking, jogging, dancing, and weightlifting are beneficial in preventing osteoporosis
- **Quit smoking and limit alcohol:** Smoking and excessive alcohol consumption can decrease bone density. Quit smoking and moderate alcohol intake to maintain bone health.
- **Regular check-ups:** Periodic check-ups with a healthcare provider can help assess bone health and determine if any preventive measures or treatments are necessary.
- **Medication:** In some cases, especially when osteoporosis is diagnosed, medication may be prescribed to slow bone loss or increase bone density. These medications should be taken under the guidance of a healthcare professional.
- **Fall prevention:** Since individuals with osteoporosis are more prone to fractures from falls, taking steps to prevent falls is crucial. This includes ensuring a safe environment at home, using assistive devices if necessary, and maintaining good balance and strength through exercise.
By incorporating these strategies into your lifestyle, you can help maintain strong and healthy bones, reducing the risk of osteoporosis and its complications.
Osteoporosis • Bone health symptoms
Osteoporosis typically doesn’t cause symptoms until a bone fracture occurs. However, when symptoms do manifest, they can include:
- **Bone fractures:** Osteoporosis weakens bones, making them more susceptible to fractures. Fractures commonly occur in the hip, spine, and wrist. Spinal fractures can lead to a stooped posture, loss of height, and back pain.
- **Back pain:** Compression fractures in the spine can cause back pain, which may be sudden and severe or develop gradually over time.
- **Loss of height:** Osteoporosis-related vertebral fractures can lead to a loss of height and a stooped posture over time.
- **Bone deformities:** Fractures in the spine can result in a forward curvature of the spine (kyphosis), leading to a hunched or stooped appearance.
- **Reduced mobility:** Fractures, particularly in the hip, can significantly reduce mobility and independence.
It’s important to note that osteoporosis can progress without any symptoms until a fracture occurs. Therefore, it’s crucial for individuals at risk to undergo regular screening and bone density tests, especially post-menopausal women and older adults. Early detection and appropriate management can help prevent fractures and maintain bone health. If you experience any of these symptoms or have concerns about your bone health, it’s essential to consult a healthcare professional for evaluation and guidance.
Osteoporosis • Bone health diagnosis
The diagnosis of osteoporosis and assessment of bone health typically involve a combination of medical history, physical examination, and specialized tests. Here’s an overview of the diagnostic process:
- **Medical History and Physical Examination:**
– Your healthcare provider will start by asking about your medical history, including any risk factors for osteoporosis such as family history, previous fractures, medications, lifestyle factors, and underlying medical conditions.
– A physical examination may be performed to assess for signs of bone loss, such as height loss, curvature of the spine, or other skeletal abnormalities with reference to osteoporosis
- **Bone Density Testing:**
– Dual-energy X-ray absorptiometry (DXA or DEXA scan) is the most commonly used test to measure bone mineral density (BMD). It involves a low-dose X-ray to measure the amount of mineral in bones, usually at the hip and spine.
– DXA results are reported as a T-score, which compares your BMD to that of a healthy young adult, and a Z-score, which compares your BMD to that of someone of your age, sex, and ethnicity.
- **Laboratory Tests:**-for osteoporosis-
– Blood tests may be ordered to measure levels of certain markers of bone turnover, such as calcium, vitamin D, parathyroid hormone (PTH), and markers of bone formation and resorption.
– These tests can help identify underlying causes of bone loss or conditions that may contribute to osteoporosis.
- **Additional Imaging Studies:**
– In some cases, additional imaging studies such as vertebral fracture assessment (VFA) may be performed to identify vertebral fractures that may not be visible on standard X-rays.
– Other imaging modalities for osteoporosis such as quantitative computed tomography (QCT) or peripheral DXA (pDXA) may be used in specific situations or for research purposes.
- **Clinical Risk Assessment Tools:**-for- osteoporosis
– Clinical risk assessment tools, such as the FRAX (Fracture Risk Assessment Tool), may be used to estimate your 10-year probability of having a major osteoporotic fracture (hip, spine, forearm) or hip fracture based on clinical risk factors and BMD measurements.
Once a diagnosis of osteoporosis is made, your healthcare provider will work with you to develop a treatment plan tailored to your individual needs, which may include lifestyle modifications, medications to prevent further bone loss or promote bone formation, and measures to reduce the risk of fractures. Regular monitoring and follow-up evaluations are essential to assess treatment effectiveness and adjust management as needed.
Osteoporosis • Bone health treatment
The treatment of osteoporosis and management of bone health aim to prevent fractures, slow bone loss, and promote bone strength. Treatment strategies may include a combination of lifestyle modifications, dietary changes, medications, and fall prevention measures. Here’s an overview:
- **Lifestyle Modifications:**
– Regular weight-bearing and muscle-strengthening exercises: Engage in activities such as walking, jogging, dancing, and weightlifting to promote bone density and strength.
– Smoking cessation: Quitting smoking can help reduce bone loss and decrease the risk of fractures due to –osteoporosis
– Limiting alcohol intake: Excessive alcohol consumption can weaken bones, so it’s important to moderate alcohol intake.
– Fall prevention: Take steps to prevent falls by ensuring a safe home environment, using assistive devices if needed, and maintaining good balance and strength through exercise.
- **Nutritional Changes:**
– Adequate calcium intake: Consume calcium-rich foods such as dairy products, leafy greens, fortified foods, and supplements if necessary. The recommended daily intake of calcium varies by age and sex.
– Sufficient vitamin D: Ensure adequate vitamin D levels through sunlight exposure, fortified foods, and supplements, as vitamin D is essential for calcium absorption and bone health and preventing osteoporosis
- **Medications:**-for –osteoporosis-
– Bisphosphonates: These drugs are often the first-line treatment for osteoporosis. They work by slowing bone loss and reducing the risk of fractures. Examples include alendronate, risedronate, and ibandronate.
– Selective estrogen receptor modulators (SERMs): Medications such as raloxifene mimic the effects of estrogen in postmenopausal women, helping to prevent bone loss and reduce fracture risk.
– Hormone therapy: Estrogen therapy may be prescribed to postmenopausal women to prevent bone loss, but it carries certain risks and is typically used for short-term management.
– Denosumab: This medication inhibits bone resorption and is administered as a subcutaneous injection every six months.
– Teriparatide and abaloparatide: These drugs are forms of parathyroid hormone that stimulate bone formation and may be prescribed for severe osteoporosis in certain cases.
- **Calcium and Vitamin D Supplements:**-for –osteoporosis-
– If dietary intake is insufficient, calcium and vitamin D supplements may be recommended to ensure adequate levels for bone health.
- **Regular Monitoring:**-for-osteoporosis
– Periodic bone density testing may be recommended to monitor response to treatment and adjust management as needed.
– Regular follow-up with a healthcare provider is important to assess treatment effectiveness, address any concerns or side effects, and make adjustments to the treatment plan as necessary.
Treatment decisions should be made in consultation with a healthcare professional, taking into account individual risk factors, preferences, and overall health status. It’s essential to adhere to the prescribed treatment regimen and attend follow-up appointments to optimize bone health and reduce the risk of fractures associated with osteoporosis.
Osteoporosis • Bone health question answer
What is osteoporosis?
Osteoporosis is a disease that thins and weakens a person’s bones. It makes them less dense and more fragile.
How can osteoporosis be prevented?
Follow a diet that has plenty of calcium and vitamin D and get regular weight-bearing exercise. These are the best ways to prevent weakened bones later in later life.
What are the warning signs of osteoporosis?
Even though osteoporosis doesn’t directly cause symptoms, you might notice a few changes in your body that can mean your bones are losing strength or density. These include:
– It might be hard to notice changes in your own physical appearance.
– A loved one may be more likely to see changes in your body (especially your height or posture).
How is osteoporosis diagnosed?
A healthcare provider will diagnose osteoporosis with a bone density test. A bone density test is an imaging test that measures the strength of your bones. It uses X-rays to measure how much calcium and other minerals are in your bones.
How is osteoporosis treated?
The most common osteoporosis treatments include:
– Exercise and making sure you get enough calcium and vitamin D in your diet.
– Your provider will help you find a combination of treatments that’s best for you and your bone health.